
Centers of Excellence
Barrett’s esophagus is a precancerous condition involving the lower portion of the esophagus. It is encountered in people suffering from gastroesophageal reflux disease (GERD). Due to the reflux, gastric acid comes back into the esophagus, irritating its walls. As a defense mechanism, the esophagus develops walls that are more resistant to acids, resembling the stomach walls. This is a precancerous condition. Out of all GERD patients 5% will develop Barrett’s esophagus and 0.3-0.5% of those patients per year will develop esophageal cancer.
For this reason, Barrett’s esophagus patients are placed on a surveillance program, usually undergoing endoscopies every 2-3 years. Biopsies are obtained during the endoscopies with the aim of early diagnosis of dysplasia or cancer.
Some key problems arise at this point:
Often dysplasia in Barrett’s esophagus is microscopic and cannot be detected by conventional endoscopes. Consequently, to this day, multiple biopsy samples are obtained during the endoscopy, in the hope of detecting potential pathological areas.
However, this entails a high margin of error, and as our team has demonstrated (Anagnostopoulos et al, Aliment Pharmacol Ther 2006) that dysplasia areas are not detected many times.
A new technique called magnification endoscopy is helpful in this regard. Magnification endoscopy inspects the esophagus wall and detects microscopic lesions in the capillary vessels, using very advanced endoscopes (image magnification x 150).
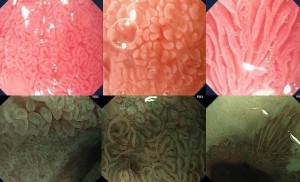
Images from files: The top row shows intestinal metaplasia in Barrett’s esophagus as seen by magnification chromoendoscopy with 1.5% acetic acid and the bottom row shows magnification endoscopy by narrow band imaging.
From the moment dysplasia is diagnosed in Barrett’s esophagus the next and most critical problem arises. What do we do?
So far, different endoscopic techniques had not provided a solution to the problem. Surgical excision of the esophagus is a radical treatment, which, nonetheless, has a 5% mortality rate even in specialized centers abroad, let alone in non-specialized centers, where this rate can be as high as 20% or more. Two new techniques have provided the solution to this point. With these techniques the pathological dysplastic area is removed and then all the Barrett’s esophagus tissue is destroyed with the help of radio waves.
Endoscopic mucosectomy is an advanced endoscopic technique that helps remove all the pathological epithelium where the dysplasia or early cancer has developed on. There are different endoscopic mucosal resection techniques.
Lately, a special plastic extension that is mounted on the tip of the endoscope and a cylindrical catheter that fits on the inside of the esophagus have been used (radiofrequency ablation – HALO system). This system blasts out energy in the form of radio waves, burning the pathological tissue to a depth that allows normal tissue regrowth and avoids the risk of perforation. The success of this technique is >90% and the complication rate is minimum.
.png)
Image: The special balloon passes through the lower esophagus, energy is released and the Barrett’s tissue is destroyed. The fact is we are entering an era where the treatment of Barrett’s esophagus is possible.
However, the major bet is to identify the GERD patient subgroup suffering from Barrett’s esophagus.